In the 1920’s, researchers at the Mayo Clinic used a ketogenic diet to treat adults with ideopathic epilepsy. In 1930, Dr. Clifford Barborka published a paper detailing their findings with their first 100 patients. Among other findings, Barborka notes that 20% of the women involved in the study experienced complete cessation of menstruation during treatment, which didn’t return until a normal diet was resumed. He only reported on menstrual cessation, but given more contemporary research on the subject we can reasonably speculate that many more women experienced menstrual irregularities that stopped short of complete cessation. Subjects were eating appropriate calories to maintain their weight, so weight loss was not a confounder here. He speculates that it may have been related to a vitamin B or E deficiency, but has no clear explanation. (Note that this was many decades before the discovery of Leptin and it’s role in hormonal regulation.)
In 2003, researchers published their retrospective study of 45 adolescents aged 12-19 treated for epilpsy with a ketogenic diet over 8 years. They noted that 45% of the girls involved in the study reported menstrual irregularities, most (2/3) of whom experienced complete cessation of menstruation (the other 1/3 were reported as experiencing delayed puberty or menstrual irregularity). Most resumed menstruation after ending the diet. 2 were treated with hormone therapy to induce and regulate menstruation. A majority of the girls did not lose weight on the diet, so again, weight loss was not a confounder in most cases. Researchers speculated that:
“The diet may mimic the menstrual side effects seen in starvation and certain female athletes.”
In 1999, a group of researchers published a review of a small group (9 women, 2 men) of otherwise healthy adults treated for epilepsy with a ketogenic diet. Of the 9 women involved in the study, 100% experienced menstrual irregularities. Although five of the 11 study subjects initially reported weight loss on the diet, calories were increased to manage it, so again, weight loss was not a confounder in most of the cases. From the researchers:
“All female patients reported menstrual irregularities. This is not uncommon, considering that menstrual irregularities are reported in other high-ketone states such as starvation.”
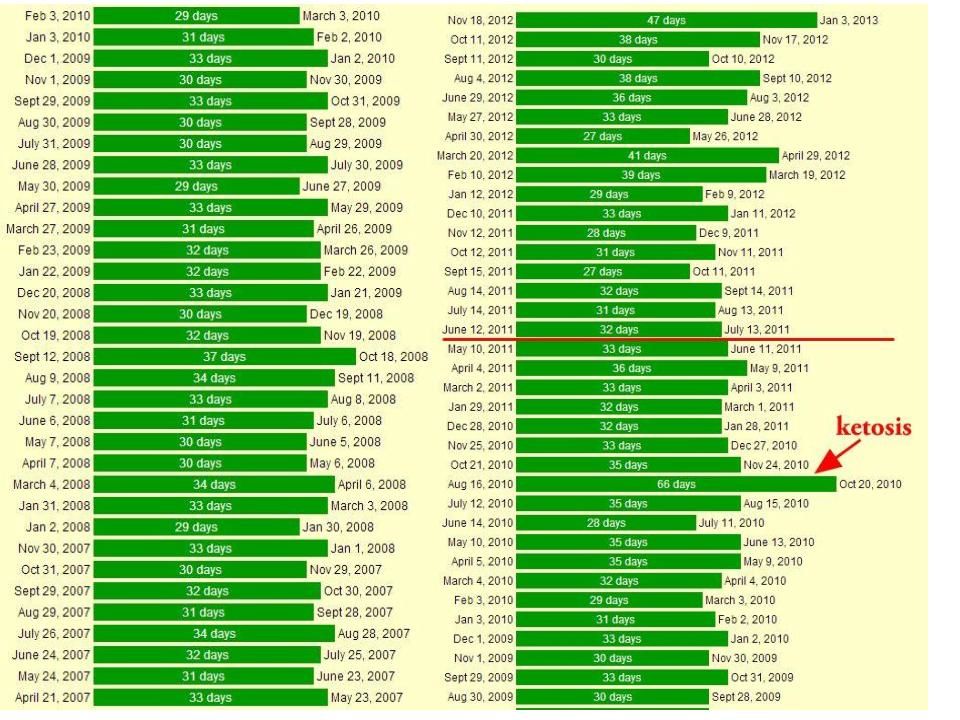
My friend Batty’s menstrual chart before (left) and after (right) experimenting with dietary restriction. Click on image to read her story.
As researchers noted, there’s some reason to speculate that the human body responds to carbohydrate restriction similarly to the way it responds to starvation. Certainly science has shown that leptin levels are sensitive to both calorie restriction (1) and carbohydrate restriction (2, 3, 4) and that women experience a greater leptin decline than men in response to dietary restriction and weight loss (5, 6). More and more research is indicating that leptin is an important endocrine mediator, acting on pituitary, adrenal, thyroid and gonadal axes, as well as playing a role in bone formation (7, 8). Another well-documented side effect of both ketogenic diets and starvation is bone demineralization (9, 10, 11, 12). Starvation and carbohydrate restriction can also both produce thyroid downregulation (13, and read Anthony Colpo’s exploration of carbohydrate restriction’s influence on thyroid function here).
I’ve worked with many women dealing with thyroid and reproductive dysfunction who also have a history of dietary restriction in the pursuit of an aesthetic ideal. My experience, coupled with the science I’ve seen, leads me to take a very cautious approach to dietary restriction in all it’s forms, with emphasis on promoting consumption of as rich a variety of calories and macronutrients as possible while allowing for the maintenance of a healthy weight. I think our culture has taken a myopic view of health, fixating on weight and fat loss, while tending to overlook other important markers of health. Most of the contemporary studies on extreme calorie and macronutrient restriction are short term, focused on only a few metabolic parameters (insulin and glucose dynamics and weight loss, most often) and/or focused on men, and I’ve found very little attention paid to leptin dynamics, thyroid health and menstrual function in the literature. The best use for highly restrictive diets are in the treatment of the illnesses they were developed to treat, and under the supervision of a qualified medical professional. For generally healthy people, a more modest, if slower, approach is probably the most prudent.
What do you do, though, if you’re already experiencing symptoms of endocrine adaptation to starvation? First of all, you may have an eating disorder, and even if you don’t you will still likely deal with issues associated with eating disorder recovery as you work your way through this stuff. Finding a medical professional with ED experience would probably be very beneficial, if for no other reason than that they can give you an idea of what to expect as your body recovers. Ask your doctor for a referral to an endocrinologist if possible. Eat! You should be eating at least as many calories as your body burns each day. If you have a history of undereating, you may need to keep track of your calorie intake to ensure it is adequate to support your energy needs. Carbs are helpful in raising leptin levels, so don’t restrict them unless you have a medical reason to and are being monitored by a medical professional. Prioritize sleep. Ask for help. You are not alone.
_____________________________________________________________________
Check out these other bloggers’ thoughts on this subject:
Krista Scott Dixon wrote an awesome post on hormones, homeostasis and carbohydrate restriction specifically in women. She touches on fasting as well.
Stafani Ruper’s discussion of carbs for health and fertility.
Danny Roddy gives a Peat‘s Eye View of female hormone regulation and provides some dietary recommendations for optimization. Of note, carbohydrates are on the menu.
Lyle McDonald’s series on leptin.
Gweneth Olwyn’s discussion of restrictive eating, leptin dynamics and infertility.
Related Posts:
Moderation is Evidence Based
Adrenal Fatigue as a Cover for Starvation
HCG, Intermittent Fasting and Ketosis
The Thing About Science
